ARTICLE Categories
All
|
|
www.facebook.com/groups/417030973601268This weeks’ article comes thanks to one of my members in my Free Facebook group for carers of children with gut and/or skin issues. She asked for exactly what it says in the title. Ideas for gently supporting gut health whilst appealing to a fussy eater.
At first glance it may appear that this article is only aimed at children, but it isn’t. You would be surprised how many adults have quite distinctive likes and dislikes when it comes to food. So, this is a great topic to tackle because it effects so many of us, whether we are a parent of a fussy eater, or whether we aren’t that keen on a few foods ourselves. Last thing before I delve properly into the topic. My belief is that fussy eaters are born and not made and so I want to take any of notion of guilt straight out of the equation. This is the little anecdote that brought me to that conclusion: My first-born loves all food, a lot. As an infant/young child he was never happier than when he was eating, and we were amazed by how adventurous he was, so young. I of course, as a first-time parent, foolishly thought that this had something to do with my parenting skills. As I was soon to find out, my son was born loving food, it had absolutely diddly squat to do with me. My daughter then arrived, and if I was a suspicious sort, I would think that she came specifically to teach me a lesson. Food didn’t interest her. She didn’t like lumps right from the start – baby porridge was a no-no, she just spat it out. She would only eat vegetables that came from tins, and she could outlast my patience at the table, by a considerable mile. She was born suspicious of most foods and there was nothing I could do to change it. Well, I did manage, but it took years. She is part of the reason I retrained as a Registered Nutritional Therapy Practitioner, I needed to know more, so I could feed her better. You’ll be pleased to hear that she now eats an amazing variety of foods and cooks for most of her friends. She still doesn’t like yogurts with ‘bits’, however. Anyway, enough digression. Today’s article is all about which nutrients are helpful to support gut health generally and some tips on how to subtlety incorporate them in the diet so that it slips past the most vigilant of fussy eaters. A quick overview of our digestive system and what it needs for health. Before we get into the nutrients and tips, just a quick overview of the gut. The gut runs all the way from our mouth to our bottom. Digestion starts in the mouth, specifically for carbohydrates (bread, pasta, flour-based products, potatoes etc), once swallowed the food passes via the oesophagus and is drip fed into the stomach. It then passes through into the small intestine, where most digestion of nutrients takes place, before moving into the large intestine where water is removed, and our gut bacteria continues to break down matter and synthesises certain vitamins. We then finally pass what’s left as a stool, and the process is complete. The whole process is managed thanks to peristalsis, a wave like action that helps propel the food to each area of the digestive stages. Many clients talk about gut problems, but that term is a little vague as issues can occur at any of the stages. We may eat too quickly and not chew enough so that the food is too large, and we experience a sensation that the food is hard to digest. We can have issues with our oesophagus so that some of the stomach acid comes up further than it should, and we experience reflux. We can have too much or even too little stomach acid so our foods, most commonly proteins, aren’t adequately broken down. We can have an issue with digestive enzymes or bile acids. Bacteria can come up to the small intestine, where they shouldn’t be and trigger small intestinal bowel overgrowth (SIBO). We can have an unbalanced gut bacteria population and constipation in the large intestine. So which nutrients are good for our digestive system? Here is a list of the nutrients, the tips on how to incorporate them will follow!
How to slip these ingredients into your fussy eater’s diet.
Sign up for my news to receive the published articles straight to your inbox. Read more by clicking below to see my previously published articles:
I’m Jessica Fonteneau, the Eczema and Digestive Health Nutrition Expert. I’ve worked with hundreds of clients to help them change their diets, better manage their flares, and find relief. My vocation is to help those with eczema and digestive issues, because I have suffered with these interlinked conditions since I was 6 months old, and I truly know what it is like to experience these debilitating conditions. Every client I have ever worked with has their own triggers and ideal nutrition. There is no such thing as ‘one-size-fits-all’. Whether you work with me one-to-one or use my guided tools, my objective is to help you uncover what works best for you, so that you take back control and experience relief. My guided programmes are only suitable for adults as children have very specific nutrition requirements. I do, however, work with many child clients as part of my clinic. I also offer two free communities for adults caring for children with eczema and digestive symptoms, feel free to come and join us and get some well-deserved support.
To easily keep up with my articles, masterclasses, ebooks and online programmes and receive exclusive access to early bird offers, sign-up to my newsletter. Interested in what I do and who I am? Go to my website: www.jessicafonteneaunutrition.com
0 Comments
Irritable bowel syndrome (IBS) is a common functional gastrointestinal condition that affects millions of people in Western societies. Incidence of IBS is on the increase with more and younger people being diagnosed and experiencing symptoms including stomach pain, bloating and irregular bowel movements. Exact causes are unknown, and IBS remains the common diagnosis once all other digestive conditions have been ruled out. Ultra-processed foods and drinks (UPFD) are increasing in both consumption and visibility, but so too is the amount of evidence growing that highlights this food group’s problematic relationship with health. This article will explore the association between consumption of UPFDs and IBS and will give 5 tips on how to transition away from UPFDs if you suffer from IBS. A quick IBS overview IBS is a complex and often long-term (chronic) digestive disorder that effects the large intestine or colon. IBS is considered a functional gut disorder as there is no damage to the gut. Symptoms can vary from person to person, but include a combination of the following:
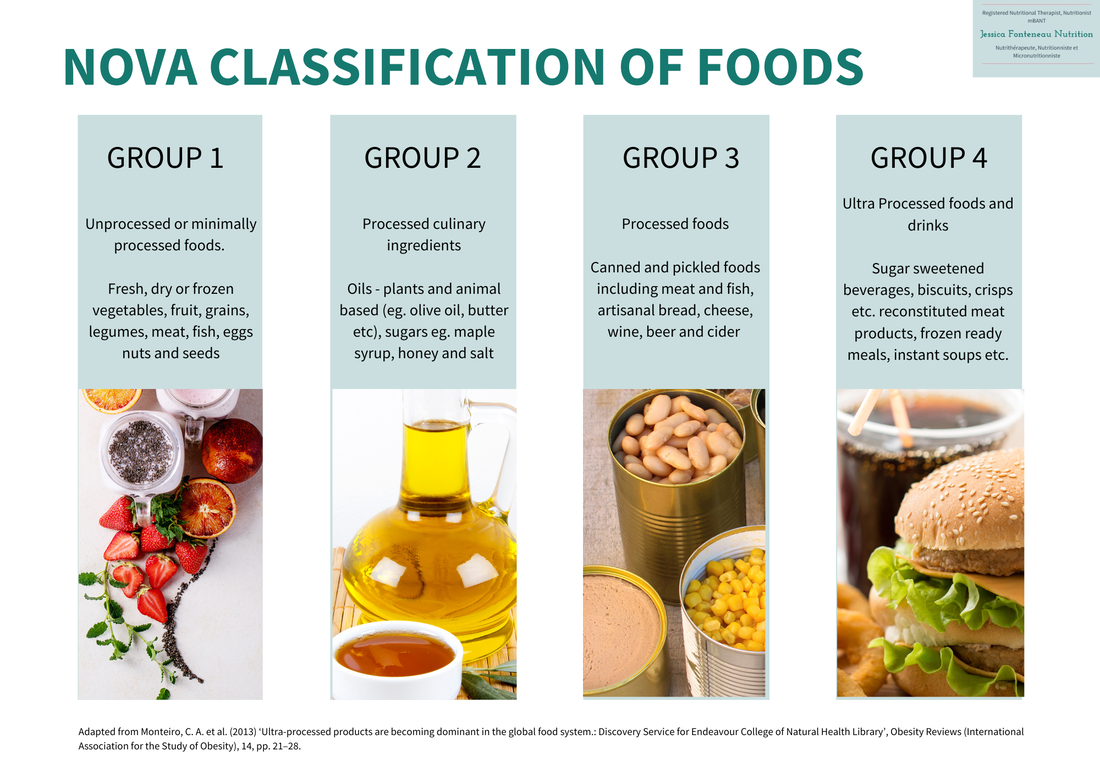
If you experience any of these symptoms, you should consult with a medical practitioner. IBS is thought to be caused by several triggers including gut motility (the movement of your stool through your gut), gut microbiome and gut hormones. Diet and stress have been identified as triggers for onset or worsening of IBS symptoms. Ultra-Processed Foods and Drinks. The jury is still out on the classification of what makes a UPFD, however since 2013 the NOVA classification developed by Monteiro et al., (6) has been the system most quoted. The NOVA classification divides products into four categories, from unprocessed or minimally processed foods to ultra-processed foods and drinks:
In a nutshell, UPFDs are highly processed products that usually contain a long list of additives, preservatives, and artificial ingredients. They can be found packaged in bright, colourful packaging and they are promoted as being convenient as well as being delicious and economical, as they usually have long shelf lives. How UPFDs affect gut health including IBS When a person is diagnosed with IBS, they are often recommended a low FODMAP diet which is fundamentally a very low fibre diet. Many of my clients come to me saying that ultra-processed foods are those that they tolerate the best on this way of eating. What they don’t realise is whilst these foods and drinks appear to be more easily digested, they are, in fact, reinforcing and exacerbating the problem. Studies have shown that the gut microbiome is different in those who regularly eat UPFDs and those that don’t. Those whose diet includes many UPFDs tend to have a larger population of gut bacteria that is considered more pro-inflammatory (triggers more inflammation). There are numerous ways in which UPFDs affect gut health and can contribute to IBS including:
5 Top Tips for Transitioning Away from Ultra-processed foods if you have IBS. Caution: someone with IBS who has been following a low FODMAP or low-fibre diet shouldn’t suddenly change their diet. I would strongly recommend that anyone wishing to modify their diet consult with a medical or nutrition practitioner.
Sign up for my news to receive the published articles straight to your inbox. Read more by clicking below to see my previously published articles:
I’m Jessica Fonteneau, the Eczema and Digestive Health Nutrition Expert. I’ve worked with hundreds of clients to help them change their diets, better manage their flares, and find relief. My vocation is to help those with eczema and digestive issues, because I have suffered with these interlinked conditions since I was 6 months old, and I truly know what it is like to experience these debilitating conditions. Every client I have ever worked with has their own triggers and ideal nutrition. There is no such thing as ‘one-size-fits-all’. Whether you work with me one-to-one or use my guided tools, my objective is to help you uncover what works best for you, so that you take back control and experience relief. My guided programmes are only suitable for adults as children have very specific nutrition requirements. I do, however, work with many child clients as part of my clinic. I also offer two free communities for adults caring for children with eczema and digestive symptoms, feel free to come and join us and get some well-deserved support.
To easily keep up with my articles, masterclasses, ebooks and online programmes and receive exclusive access to early bird offers, sign-up to my newsletter. References
There comes a time in most parent’s life when you are faced with your child complaining of stomach-ache and asking to stay home from school. I know, it happened to me frequently with my youngest daughter.
It can be so hard to judge, especially with younger children, whether the issue is serious or simply an appeal for a day off. My daughter has admitted that some of those earlier episodes were a case of her just wanting to stay home rather than face a test, but others were genuine. When her stomach aches started to interfere with her high-level sport practice, which she loved, I knew for sure that things weren’t right, and I consulted our GP who referred her to a gastroenterologist. In her case, all was well, but if you have any doubt about your child’s symptoms, consult your own medical practitioner. Whilst children’s stomach aches can be triggered by many things, for some it comes from Paediatric Irritable Bowel Syndrome (IBS) and this article will give an overview on:
Understanding paediatric IBS IBS, whether paediatric or adult, is a functional gastrointestinal disorder. That means that there is no physical damage to the gut, but rather a disorder in how the digestive system is working, which can lead to a range of distressing symptoms. Paediatric IBS often develops during adolescence, but some children develop the condition at a younger age. It is thought that up to 15% of the paediatric population suffers from this condition. The name Irritable Bowel Syndrome (IBS) can easily be confused with Irritable Bowel Disease (IBD) which encompasses Crohn’s and Ulcerative Colitis, but it is a completely different condition. Symptoms of paediatric IBS
Diagnosing paediatric IBS Any children with persistent symptoms should see their medical practitioner. It is worth being aware that diagnosing paediatric IBS can be challenging, because it overlaps with other gastrointestinal disorders, and it is usually diagnosed following a process of elimination via a combination of medical history, physical examination, and tests. If your family has any history of gastrointestinal disorders, then it is essential to share that information with your medical practitioner. Tips for how to support your child diagnosed with IBS.
IBS in children is a real, but often misunderstood condition that can have a significant impact on a child’s daily life. Recognising the symptoms, seeking healthcare advice for proper diagnosis and nutrition support, and introducing some anxiety relief techniques are crucial to help improve quality of life. Sign up for my news to receive the published articles straight to your inbox. Read more by clicking below to see my previously published articles:
I’m Jessica Fonteneau, the Eczema and Digestive Health Nutrition Expert. I’ve worked with hundreds of clients to help them change their diets, better manage their flares, and find relief. My vocation is to help those with eczema and digestive issues, because I have suffered with these interlinked conditions since I was 6 months old, and I truly know what it is like to experience these debilitating conditions. Every client I have ever worked with has their own triggers and ideal nutrition. There is no such thing as ‘one-size-fits-all’. Whether you work with me one-to-one or use my guided tools, my objective is to help you uncover what works best for you, so that you take back control and experience relief. My guided programmes are only suitable for adults as children have very specific nutrition requirements. I do, however, work with many child clients as part of my clinic. I also offer two free communities for adults caring for children with eczema and digestive symptoms, feel free to come and join us and get some well-deserved support.
To easily keep up with my articles, masterclasses, ebooks and online programmes and receive exclusive access to early bird offers, sign-up to my newsletter. Foods, ingredients, or molecule intolerances appear to be on the rise and whilst some such as gluten or histamine are well known, others, such as salicylates, are more misunderstood. This article will delve into this lesser-known phenomenon exploring:
What are salicylates and what is a salicylate intolerance? Salicylates are natural chemicals found in many plants who use them to defend themselves against pests, bacteria, and environmental stressors. Salicylates are anti-inflammatory and as such have also been synthetically reproduced in laboratories for uses in medications, including aspirin and non-steroidal anti-inflammatories (NSAIDs) such as ibuprofen. Salicylic acid has excellent anti-fungal and anti-bacterial properties, leading to its common use as an ingredient in processed foods, condiments, cosmetics, and beauty products. In terms of food, salicylates are found in many plant foods to a higher or lesser extent. Some of the foods that are common triggers are:
Salicylate intolerance is where a person’s system has difficulty metabolising and tolerating salicylates, leading to a range of symptoms. The phenomenon was initially observed in medically diagnosed patients with either aspirin-exacerbated respiratory disease (AERD) or NSAIDs-exacerbated respiratory disease (NERD) (1,2). In the cases of both AERD and NERD, high doses of chemical salicylates can trigger asthma, rhinosinusitis and urticaria. Clinical case studies have observed that for some, simply eating a diet high in salicylates can contribute to a variety of symptoms, although this can vary from person to person and may also depend on the quantity of salicylates eaten or exposed to over a short period of time. Which symptoms are linked to salicylate intolerance? Whilst respiratory and skin symptoms are the most recognised symptoms of salicylate intolerance, there are others including:
What does the science say causes this condition? As with so many conditions, the exact cause of salicylate intolerance is not well understood, however there are some areas which are being explored:
How is salicylate intolerance medically diagnosed? Diagnosis of salicylate intolerance is tricky, mainly because of the number of overlapping symptoms with other conditions. A medical or nutrition practitioner will undertake:
For many, a salicylate intolerance is linked to other conditions or genetics and is not, itself, the root cause. Sufferers tend to go heavily down the elimination root, which whilst does initially provide relief, is not a sustainable or healthy long-term solution. Working with a practitioner to discover the main trigger of the sensitivity is key. Suggestions for managing a suspected salicylate intolerance.
If on medication, please speak to your GP/consultant before making any changes to your diet. Sign up for my news to receive the published articles straight to your inbox. Read more by clicking below to see my previously published articles:
I’m Jessica Fonteneau, the Eczema and Digestive Health Nutrition Expert. I’ve worked with hundreds of clients to help them change their diets, better manage their flares, and find relief. My vocation is to help those with eczema and digestive issues, because I have suffered with these interlinked conditions since I was 6 months old, and I truly know what it is like to experience these debilitating conditions. Every client I have ever worked with has their own triggers and ideal nutrition. There is no such thing as ‘one-size-fits-all’. Whether you work with me one-to-one or use my guided tools, my objective is to help you uncover what works best for you, so that you take back control and experience relief. My guided programmes are only suitable for adults as children have very specific nutrition requirements. I do, however, work with many child clients as part of my clinic. I also offer two free communities for adults caring for children with eczema and digestive symptoms, feel free to come and join us and get some well-deserved support.
To easily keep up with my articles, masterclasses, ebooks and online programmes and receive exclusive access to early bird offers, sign-up to my newsletter. Interested in what I do and who I am? Go to my website: www.jessicafonteneaunutrition.com References:
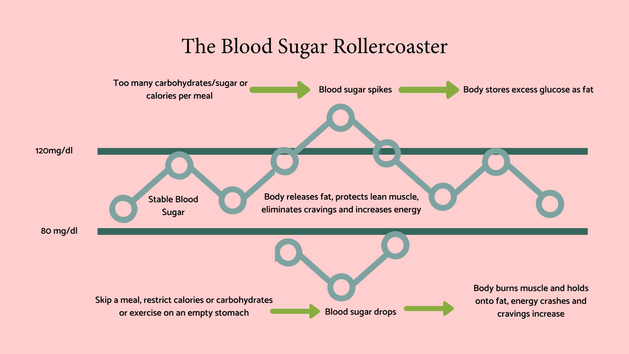
Blood sugars and continuous blood sugar monitors are all the rage and for good reason. Maintaining a stable blood sugar level isn’t just vital for metabolic health and weight, but also plays a key role in maintaining healthy skin and a normal functioning gut. This article will explore the connections between stable blood sugars and both skin and gut health and will provide practical tips to achieve and maintain this important balance:
The role of stable blood sugars Before we go into the detail of blood sugar and skin and gut health, here’s a quick overview of how important blood sugars are, so that we put it all in context. Simplistically, blood sugar is our main source of energy, and we get it primarily from eating carbohydrates which our digestive system then breaks down to glucose. This then enters our blood stream and provides energy to cells. Stable blood sugars are vital for lots of reasons, but here are the most cited ones:
Blood sugars and skin health
There are several ways that blood sugars can have an impact on skin health including:
Blood sugars and gut health Blood sugars and gut health aren’t usually associated by most people; however, high blood sugar levels can influence:
My top tips for keeping your blood sugars stable.
I run a 5 day ‘A Week to Reduce Your Sugar Cravings’ Challenge – it’s absolutely free and you can sign up here. Sign up for my news to receive the published articles straight to your inbox. Read more by clicking below to see my previously published articles:
I’m Jessica Fonteneau, the Eczema and Digestive Health Nutrition Expert. I’ve worked with hundreds of clients to help them change their diets, better manage their flares, and find relief. My vocation is to help those with eczema and digestive issues, because I have suffered with these interlinked conditions since I was 6 months old, and I truly know what it is like to experience these debilitating conditions. Every client I have ever worked with has their own triggers and ideal nutrition. There is no such thing as ‘one-size-fits-all’. Whether you work with me one-to-one or use my guided tools, my objective is to help you uncover what works best for you, so that you take back control and experience relief. My guided programmes are only suitable for adults as children have very specific nutrition requirements. I do, however, work with many child clients as part of my clinic. I also offer two free communities for adults caring for children with eczema and digestive symptoms, feel free to come and join us and get some well-deserved support.
To easily keep up with my articles, masterclasses, ebooks and online programmes and receive exclusive access to early bird offers, sign-up to my newsletter. Interested in what I do and who I am? Go to my website: www.jessicafonteneaunutrition.com References:
Histamine intolerance is a recently identified but increasingly considered condition that, whilst not life-threatening, can trigger a range of uncomfortable and often debilitating symptoms. The disparity and variety of symptoms that can be attributed to this condition are so widespread that it took time for the scientific community to observe the common denominator, and it is often misdiagnosed in general practice. This, the fifth and last article in my ‘histamine’ series, will delve into this condition that is grabbing the attention of the healthcare community, providing you with information that may help you unravel whether histamine intolerance may be a factor in your health. The article covers:
What is histamine intolerance? Histamine intolerance, also known as histaminosis or histamine sensitivity, is an increasingly recognised condition that affects a significant number of people worldwide. (1,2) is usually defined as the inability to adequately breakdown histamine. Histamine is a neurotransmitter, found throughout the body, but specifically in the skin, respiratory tract, and the digestive system. It is involved in numerous processes including stomach acid production, and vasodilation (the widening of the blood vessels), but is more commonly known for its pivotal involvement in the immune response. It is believed that individuals who suffer from histamine intolerance have a deficiency or dysfunction of the DAO (diamine oxidase) or HNMT (histamine-N-methyltransferase, enzymes, which are responsible for breaking down histamine in the body. This slowing of histamine degradation leads to a possible accumulation of histamine, leading to a variety of symptoms, depending on the individual. It is thought that histamine intolerance prevalence is higher in children than in adults (3), but further studies are needed. My clinical experience, working with many infants and young children with digestive and skin symptoms, is that when true IgE allergies have been ruled out, histamine intolerance is often a route to be explored. Lowering an overall histamine load, rather than assuming that multiple food intolerances are at play, can allow children to retain the all-important macro and micronutrient variety, rather than putting them at risk of strict and restrictive elimination diets which oftentimes worsens the situation and puts their health at risk. Histamine intolerance has, in the past, often been misdiagnosed as whole host of other diseases including food allergy and intolerances, urticaria, eosinophilic gastroenteritis amongst others. When clients come to see me with negative allergy/intolerance testing, but who swear blind that such and such a food triggers a reaction, histamine intolerance is something that immediately springs to mind. Which symptoms hint at a possible histamine intolerance? As I’ve already explored in previous articles (see links at the end of this feature), histamine intolerance can manifest in a variety of different symptoms, hence the diagnosis difficulty. Common symptoms include:
What are the possible contributory causes? There are several possible contributory causes to histamine intolerance, but the main theory involves the concept of an overall histamine ‘load’ or the cumulative effect of several factors, including:
Please note that not every individual will be affected by all the above, and this overview should only support the notion of how your overall histamine load could add up. The genetics of histamine intolerance For some experiencing histamine issues, the question of low or slow DAO or HNMT activity may stem from their genetics. DAO inactivates histamine in the gut and HNMT within the nervous system and lungs. Genetic variants on these enzymes or their pathways can lead to histamine intolerance. Nutrigenomics testing, which I offer through Lifecode Gx, can provide information on our own genes which then informs us on the nutrition and lifestyle changes we can make to align with any variants to optimise health and wellbeing. Lifecode Gx offers a specific Histamine Intolerance test. You can find out more, by clicking the link. Nutrigenomic testing is the only form of testing that is available from the youngest age. Whilst how you eat and live your life will have an effect on whether a gene variation may have an impact, your genes themselves never change. My top tips for lowering your histamine load.
If on medication, please speak to your GP/consultant before making any changes to your diet. If you are interested in histamine and its impact on symptoms, this article is the second in a series I am currently publishing covering. The series in total will include:
Sign up for my news to receive the published articles straight to your inbox. Read more by clicking below to see my previously published articles:
I’m Jessica Fonteneau, the Eczema and Digestive Health Nutrition Expert. I’ve worked with hundreds of clients to help them change their diets, better manage their flares, and find relief. My vocation is to help those with eczema and digestive issues, because I have suffered with these interlinked conditions since I was 6 months old, and I truly know what it is like to experience these debilitating conditions. Every client I have ever worked with has their own triggers and ideal nutrition. There is no such thing as ‘one-size-fits-all’. Whether you work with me one-to-one or use my guided tools, my objective is to help you uncover what works best for you, so that you take back control and experience relief. My guided programmes are only suitable for adults as children have very specific nutrition requirements. I do, however, work with many child clients as part of my clinic. I also offer two free communities for adults caring for children with eczema and digestive symptoms, feel free to come and join us and get some well-deserved support.
To easily keep up with my articles, masterclasses, ebooks and online programmes and receive exclusive access to early bird offers, sign-up to my newsletter. Interested in what I do and who I am? Go to my website: www.jessicafonteneaunutrition.com References:
Upcoming programmes and eventsClick on the thumbnails to find out more
It’s a fascinating fact that before puberty, if you are born male, you are more at risk from childhood allergies, but that after puberty those born female are more likely to suffer from conditions relating to immune function including allergies and autoimmune conditions. (1,2)
It’s also reported that many people experience an onset, worsening or sometimes remission from eczema and IBS symptoms at certain times in the menstrual cycle or life stage e.g. pregnancy and menopause. Have you ever considered why? Studies have hinted at the interaction of the neurotransmitter, histamine, and the hormones, oestrogen, and progesterone. Today’s article, the fourth in my ‘histamine’ series, explores this emerging topic and includes:
Histamine, a quick overview Histamine is a compound that acts as both a neurotransmitter and an immune system messenger. It is responsible for a range of roles, including immune response, vasodilation (the widening of the blood vessels), and stomach acid production. Whilst histamine is vital for protecting the bodies against infection and supporting wound healing, too much histamine can lead to various health issues. For more detail on how this might link to digestive health, skin conditions or autoimmunity, please see my previous articles, links below. Oestrogen, progesterone, and the menstrual cycle The menstrual cycle is an intricate ballet of hormonal fluctuations, depending on distinct phases, going from menstruation to the follicular phase, ovulation and finally the luteal phase. During this cycle levels of sex hormones, including oestrogen, progesterone, luteinising hormone, and follicular stimulating hormone, rise and fall with the aim to prepare the body for pregnancy. Oestrogen is a group of sex hormones (estrone, oestradiol and estriol) that plays a key role in the development and functioning of the female reproductive system. Less well considered is the fact that oestrogen also impacts bone health, cardiovascular function, cognitive function, and the modulation of the immune system. Oestrogen levels are at their highest during the follicular phase, between the first day of a period and the next ovulation (days 1-14). Oestrogen is primarily excreted from the body following detoxification via the liver. Some oestrogen is, however, recycled and remains in circulation which may lead to oestrogen levels being proportionately higher at some times. Progesterone, another vital hormone, works in step with oestrogen to regulate the menstrual cycle and prepare the body for a potential pregnancy. It also plays a role in thermoregulation (cooling you down or keeping your warm), skin health, brain function, and vitally has anti-inflammatory actions. Progesterone levels are highest during the Luteal phase of your cycle. This is the phase directly after ovulation which lasts until your next cycle begins. Oestrogen, progesterone, and histamine, how might they interact? Research suggests that histamine levels are influenced by the hormonal fluctuations that happen during the menstrual cycle. Oestrogen has been demonstrated to encourage release of histamine from mast cells. This may explain the increase in symptoms such as allergies, migraines and eczema during the follicular phase, reported by many. (1) Some studies, have indicated that oestrogen may not just trigger mast cells to produce histamine but may also downregulate the production of DAO (diamine oxidase), one of the enzymes that breaks down histamine in the gut. (3,4) Some studies suggest that progesterone may slow mast cells from releasing histamine. (5) Histamine levels linked to the menstrual cycle. A useful, but basic summary, particularly in relation to the topic we are discussing today is the fact that oestrogen can stimulate histamine production and progesterone is anti-inflammatory. If we know that oestrogen levels are highest during the follicular phase and progesterone’s are highest in the luteal phase, then we can start to consider whether a person’s own symptoms can be mapped to their cycle. It is important to note that whilst some do report an increased sensitivity to histamine during certain phases of their cycle, many do not. Histamine and pregnancy Hormone levels are increased during pregnancy and for those sensitive to histamine, an increase in skin or digestive issues may be experienced at that time. Morning sickness can also be related to histamine’s role in stomach acid production. On the other hand, during pregnancy the immune system is naturally heightened, which for some results in remission from eczema or other symptoms for the duration of the pregnancy. Menopause and histamine imbalance The menopause marks the end of the reproductive years and is characterised by a host of hormonal changes including the reduction of oestrogen and the almost total cessation of progesterone production. Remember, oestrogen can induce histamine production whereas progesterone counter acts the effect with its anti-inflammatory role. So, during the menopause when progesterone levels are almost nil, but oestrogen continues to be produced, the scene is set for histamine load to be higher, and many menopause symptoms are directly related to this, including:
My recommendations for keeping histamine in check.
If on medication, please speak to your GP/consultant before making any changes to your diet. If you are interested in histamine and its impact on symptoms, this article is the second in a series I am currently publishing covering. The series in total will include:
Sign up for my news to receive the published articles straight to your inbox. Read more by clicking below to see my previously published articles:
I’m Jessica Fonteneau, the Eczema and Digestive Health Nutrition Expert. I’ve worked with hundreds of clients to help them change their diets, better manage their flares, and find relief. My vocation is to help those with eczema and digestive issues, because I have suffered with these interlinked conditions since I was 6 months old, and I truly know what it is like to experience these debilitating conditions. Every client I have ever worked with has their own triggers and ideal nutrition. There is no such thing as ‘one-size-fits-all’. Whether you work with me one-to-one or use my guided tools, my objective is to help you uncover what works best for you, so that you take back control and experience relief. My guided programmes are only suitable for adults as children have very specific nutrition requirements. I do, however, work with many child clients as part of my clinic. I also offer two free communities for adults caring for children with eczema and digestive symptoms, feel free to come and join us and get some well-deserved support.
To easily keep up with my articles, masterclasses, ebooks and online programmes and receive exclusive access to early bird offers, sign-up to my newsletter. Interested in what I do and who I am? Go to my website: www.jessicafonteneaunutrition.com References:
Histamine is often thought of in relation to hay fever and skin reactions, such as atopic eczema, but did you know that histamine is also implicated in digestive health conditions including reflux, irritable bowel syndrome (IBS) and Inflammatory Bowel Disease (IBD)?
Today’s article, the second in the series, focuses on histamine and its link to gut health and includes:
What role does histamine play in digestion? Histamine, a neurotransmitter, and immune system mediator, plays a crucial role in a whole range of processes and is found throughout the body, including the gastrointestinal tract. Histamine is released by mast cells and basophils in response to allergens, pathogens, tissue damage, amongst other stimuli and plays a dual role in the digestive system, at times being pro-inflammatory and at others anti-inflammatory. It has several roles including (1):
Which digestive disorders are linked to histamine?
What are the possible triggers of a histamine reaction in the gut?
In summary, here are my top tips for managing histamine as a trigger for gut disorders:
If on medication, please speak to your GP/consultant before making any changes to your diet. If you are interested in histamine and its impact on symptoms, this article is the second in a series I am currently publishing. The series will include:
Sign up for my news to receive the published articles straight to your inbox. Read more by clicking below to see my previously published articles:
I’m Jessica Fonteneau, the Eczema and Digestive Health Nutrition Expert. I’ve worked with hundreds of clients to help them change their diets, better manage their flares, and find relief. My vocation is to help those with eczema and digestive issues, because I have suffered with these interlinked conditions since I was 6 months old, and I truly know what it is like to experience these debilitating conditions. Every client I have ever worked with has their own triggers and ideal nutrition. There is no such thing as ‘one-size-fits-all’. Whether you work with me one-to-one or use my guided tools, my objective is to help you uncover what works best for you, so that you take back control and experience relief. My guided programmes are only suitable for adults as children have very specific nutrition requirements. I do, however, work with many child clients as part of my clinic. I also offer two free communities for adults and adults caring for children with eczema and digestive symptoms, feel free to come and join us and get some well-deserved support.
To easily keep up with my articles, masterclasses, ebooks and online programmes and receive exclusive access to early bird offers, sign-up to my newsletter. Interested in what I do and who I am? Go to my website: www.jessicafonteneaunutrition.com References: 1. Chen M, Ruan G, Chen L, Ying S, Li G, Xu F, et al. Neurotransmitter and Intestinal Interactions: Focus on the Microbiota-Gut-Brain Axis in Irritable Bowel Syndrome. Front Endocrinol (Lausanne). 2022;13(February):1–12. 2. Rettura F, Bronzini F, Campigotto M, Lambiase C, Pancetti A, Berti G, et al. Refractory Gastroesophageal Reflux Disease: A Management Update. Front Med. 2021;8(November):1–19. 3. Zaterka S, Marion SB, Roveda F, Perrotti MA, Chinzon D. Historical perspective of gastroesophageal reflux disease clinical treatment. Arq Gastroenterol. 2019;56(2):202–8. 4. Melgarejo E, Medina MÁ, Sánchez-Jiménez F, Urdiales JL. Targeting of histamine producing cells by EGCG: a green dart against inflammation? J Physiol Biochem [Internet]. 2010;66(3):265–70. Available from: https://doi.org/10.1007/s13105-010-0033-7 5. Kanikowska A, Janisz S, Mańkowska-Wierzbicka D, Gabryel M, Dobrowolska A, Eder P. Management of Adult Patients with Gastrointestinal Symptoms from Food Hypersensitivity—Narrative Review. Vol. 11, Journal of Clinical Medicine. 2022. Every so often a new health buzz word emerges. The new “thing” that, once resolved, will, theoretically, solve everything.
From the questions I get within my community forums or from clients, histamine seems to be the current molecule of interest, particularly in relation to skin, gut and autoimmune issues, but does it deserve this notoriety? There is a lot to unpick regarding histamine, so I have divided the topic into 5 separate articles. The first is published below and the next four will follow over the next month, so keep watching this space or sign-up for my emails to receive the articles direct to your inbox:
What is the histamine and eczema/dermatitis link? Today’s article covers:
What is histamine? Histamine is a neurotransmitter, produced by mast cells, found throughout the body, but specifically in the skin, respiratory system, and the gastrointestinal tract, but also by basophils, a type of white blood cell which is involved in an immune reaction. Histamine is mostly known for its involvement in the immune response cascade (one reaction, causing the next and so on). This neurotransmitter is directly responsible for itching, redness and swelling (inflammation) but is also involved in numerous other processes including stomach acid, contraction of smooth muscle (muscles involved with respiration and digestion amongst others), and the dilation of blood vessels. Whilst histamine, the neurotransmitter, is the main driver, there are four different types of histamine receptors (H Receptors) which determine the type or location of a histamine response. (2,3)
Histamine and the immune system, how does it work? When the body encounters an allergen, be it environmental (pollen or dust mites, for example) or food (e.g., gluten, dairy etc.) the immune system responds by producing immunoglobulin E (IgE) antibodies which bind to mast cells and basophils which then trigger the release of histamine. Histamine release makes blood vessels dilate resulting in blood rushing to the area and leading to the common signs of inflammation: redness, itching and swelling. Histamine is also involved in the inflammatory response when tissue (or skin) is damaged or infected, causing the blood vessels dilate, drawing blood flow and delivering white blood cells to the damaged area which then help to fight off possible infection. Histamine and eczema/dermatitis – what is the link? Atopic Eczema alone affects an estimated 20% of children and 10% of adults in the Western world (1), which is an absolutely massive number of people. If you suffer from any type of eczema/dermatitis you already know that it is a chronic inflammatory skin condition that can be dry, itchy, and inflamed, all symptoms linked to a histamine response. Most researchers agree that there is a link between histamine and eczema/dermatitis. Histamine triggers inflammation, causing itchiness, redness, swelling and testing has identified that individuals suffering from an eczema/dermatitis flare, have high levels of histamine. What is less clear is what the specific connection is. In other words, just as no two eczema/dermatitis sufferers appear to have the same triggers, the histamine connection may be different for everyone. In terms of current and recent research, the following three links have been specifically examined:
Research suggests that histamine’s role in eczema/dermatitis may go beyond its inflammatory role. Evidence has been found that it may contribute to the breakdown of the skin barrier, resulting in ‘Leaky Skin’, making skin less able to retain moisture and act as a protection against irritants. This means that potential allergens and irritants cross into the body more easily, triggering an immune response. Exploring the eczema types most linked to histamine. As we already know, not all eczema/dermatitis is alike, which means that not all types will necessarily have a histamine link, but those that are include:
In summary, here are my 7 top tips for managing histamine as a trigger for eczema/dermatitis:
Speak to your medical practitioner, Registered Nutritional Therapist or pharmacist adviser for further guidance. If on medication, please speak to your GP/consultant before making any changes to your diet. Histamine Masterclass - 1pm, Thursday 14th September. I will be holding an online Masterclass on histamine on Thursday 14th September 2023 at 1pm - claim your early bird ticket at £10. Don't worry if you can't attend live, you can send your questions in advance and the Masterclass will be emailed to all attendees post the event. Read more:
Interested in what I do and who I am? Go to my website: www.jessicafonteneaunutrition.com 1. Nutten S. Atopic dermatitis: Global epidemiology and risk factors. Ann Nutr Metab. 2015;66:8–16. 2. Buddenkotte J, Maurer M, Steinhoff M. Histamine and antihistamines in atopic dermatitis. Adv Exp Med Biol. 2010;709:73–80. 3. Patel RH; Mohiuddin SS. Biochemistry , Histamine. 2023;32491722. |
AuthorI’m Jessica Fonteneau, I’m the eczema specialist and I help people Escape from the Eczema trap. Archives
April 2024
Catégories
All
|






















 RSS Feed
RSS Feed